- Research
- /
- PRECOGNIZE study
PRECOGNIZE study
Supporter
National Brain Research Programme II (2017-1.2.1-NKP-2017-00002)
Research leader
Prof. Dr. Anita Kamondi and Precognize Ltd.
Duration
2017- indefinite
Háttér:
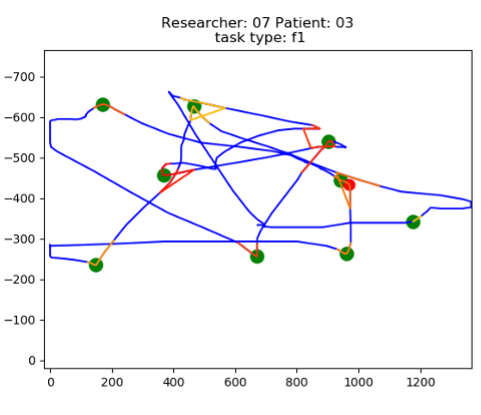
In the early stages of Alzheimer's disease, according to the Braak stages, amyloid deposition in the brain region around the hippocampus is the characteristic pathological abnormality, and accordingly the clinical picture does not yet show the symptoms that are most commonly evaluated, memory complaints. However, outside the temporal lobe region, prominent abnormalities are already detectable, particularly in the prefrontal and posterior parietal cortical areas. Since associative functioning between these areas is essential during planned eye-hand coordination activities, it is assumed that deficit-level involvement of these functions can be detected at an early stage. These hypotheses are in line with the modern view of Alzheimer's disease, in which primary pathological and clinical abnormalities can be detected up to decades before the onset of initial, subjective memory complaints. The clinical symptoms may be primarily due to a loss of associative function between different cortical areas, which is the basis for the theory of Alzheimer's disease as a disconnective oscillopathy. In the light of the above findings, computerized eye-hand coordination testing (e.g. cursor movements) may be useful to clarify the diagnosis of AD, to improve the differential diagnostic efficiency of dementias and to screen for mild cognitive impairment. It is hoped that the disease could thus be detected even by screening in general practice, before the representation of primary clinical symptoms.
Last updated: 06.06.2021.